About Behavioral Health

California has a behavioral health care crisis, as more Californians need care, and there are not enough providers to deliver that care. As a last resort, those facing a mental health crisis turn to hospital emergency departments. The number of people going to an emergency department for mental health needs jumped 68% from 2010 to 2020; for children 12 to 17 that number climbed 31%. Creating a behavioral health care system means making access easier and more equitable, while ensuring patients receive care in the most appropriate setting.
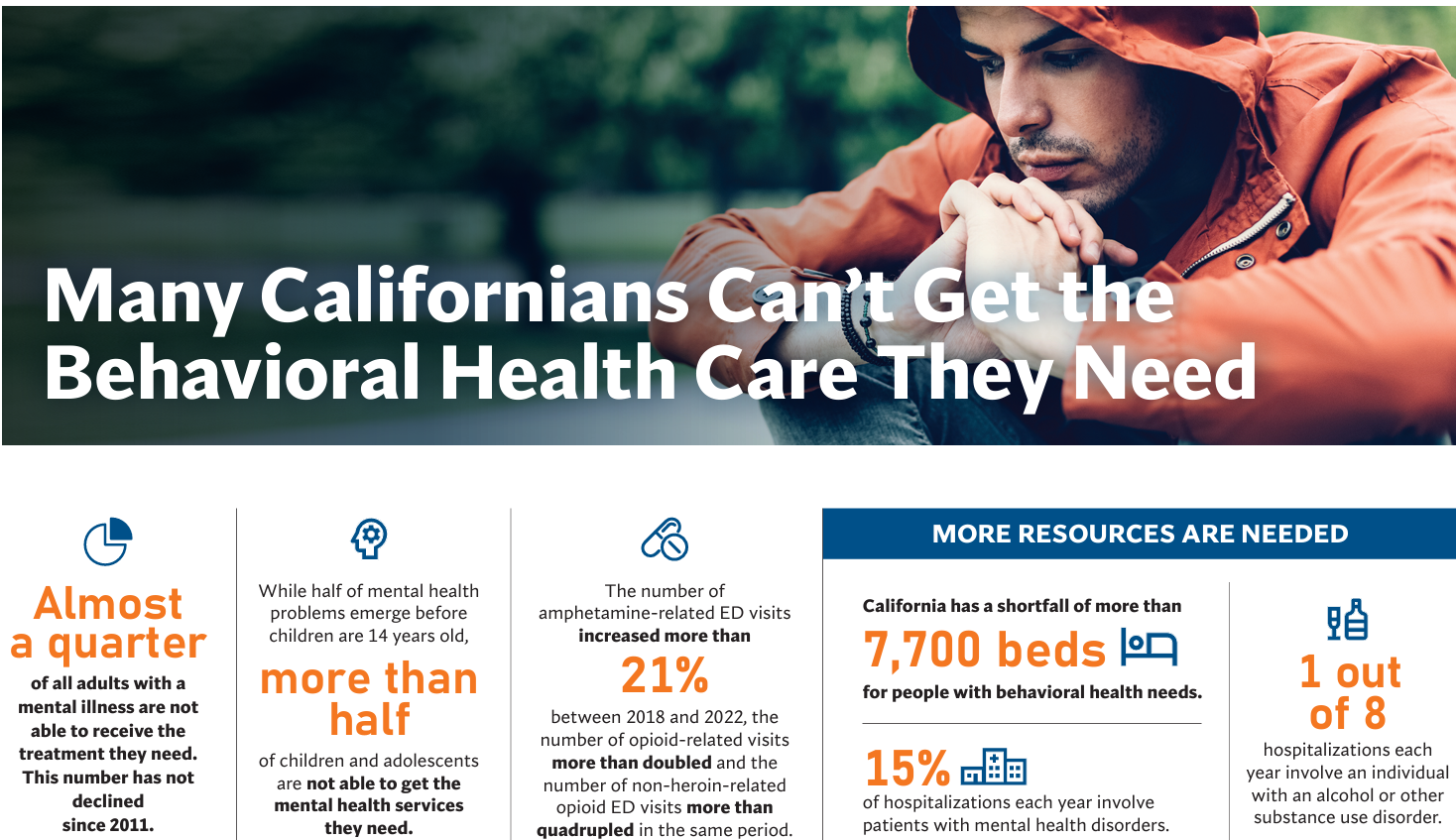
Infographic: The Facts About Behavioral Health Care
Issue Brief: Steps to Address Behavioral Health Care Challenges
Solutions must mirror those in primary care, where the goal is to prevent illness and provide the right care in the right setting.
Key Messages: Learn What’s Driving Challenges in Behavioral Health Care
Due to a shortage of behavioral health resources, many Californians struggle to find the treatment they need.
Children’s Behavioral Health Services Lack Timely Access
What’s happening: The California State Auditor recently investigated children’s access to Medi-Cal-covered behavioral health services.
What else to know: The auditor concluded that many Medi-Cal health plans were out of compliance with state requirements for timely care and that the Department of Health Care Services (DHCS) is not adequately disciplining health plans.
2023 Behavioral Health Care Symposium Will Be Held in Sacramento for First Time
What’s happening: For the first time, CHA’s 2023 Behavioral Health Care Symposium (Dec. 12-13) will be held in Sacramento and have a heavy legislative focus.
What else to know: The keynote speaker will be Sen. Susan Talamantes Eggman, (D-Stockton), chair of the Senate Health Committee and a leader on behavioral health in the Legislature.
Continuing Education Credits Available in Multiple Areas for Symposium Attendees
What’s happening: CHA’s 2023 Behavioral Health Care Symposium (Dec. 12-13) in Sacramento will offer continuing education (CE) credits in multiple areas for qualifying participants.
What else to know: To qualify to receive CE credits, registrants must complete a post-event survey, attest to participation, and provide a professional license number.
2023 Legislative Wrap-Up
Access to Mental Health Services Could Increase for Medicare Advantage Enrollees
What’s happening: The Centers for Medicare & Medicaid Services (CMS) proposes policy changes for Medicare Advantage (MA) plans in contract year (CY) 2025.
What else to know: Comments on the proposed rule, which addresses MA policies such as prior authorization, outpatient behavioral health and supplemental benefits, are due Jan. 5.
Senator Susan Talamantes Eggman will open the Symposium as the Keynote
Why you should attend: Hear from Sen. Susan Talamantes Eggman, a leader on behavioral health in the Legislature, and get an update on public policies, politics, and financial issues shaping behavioral health care in California.
When: Dec. 12-13 at the Kimpton Sawyer Hotel in Sacramento.